The Ultimate Choice for Ultimate Spine SolutionsTM
Virginia Spine Institute is now VSI
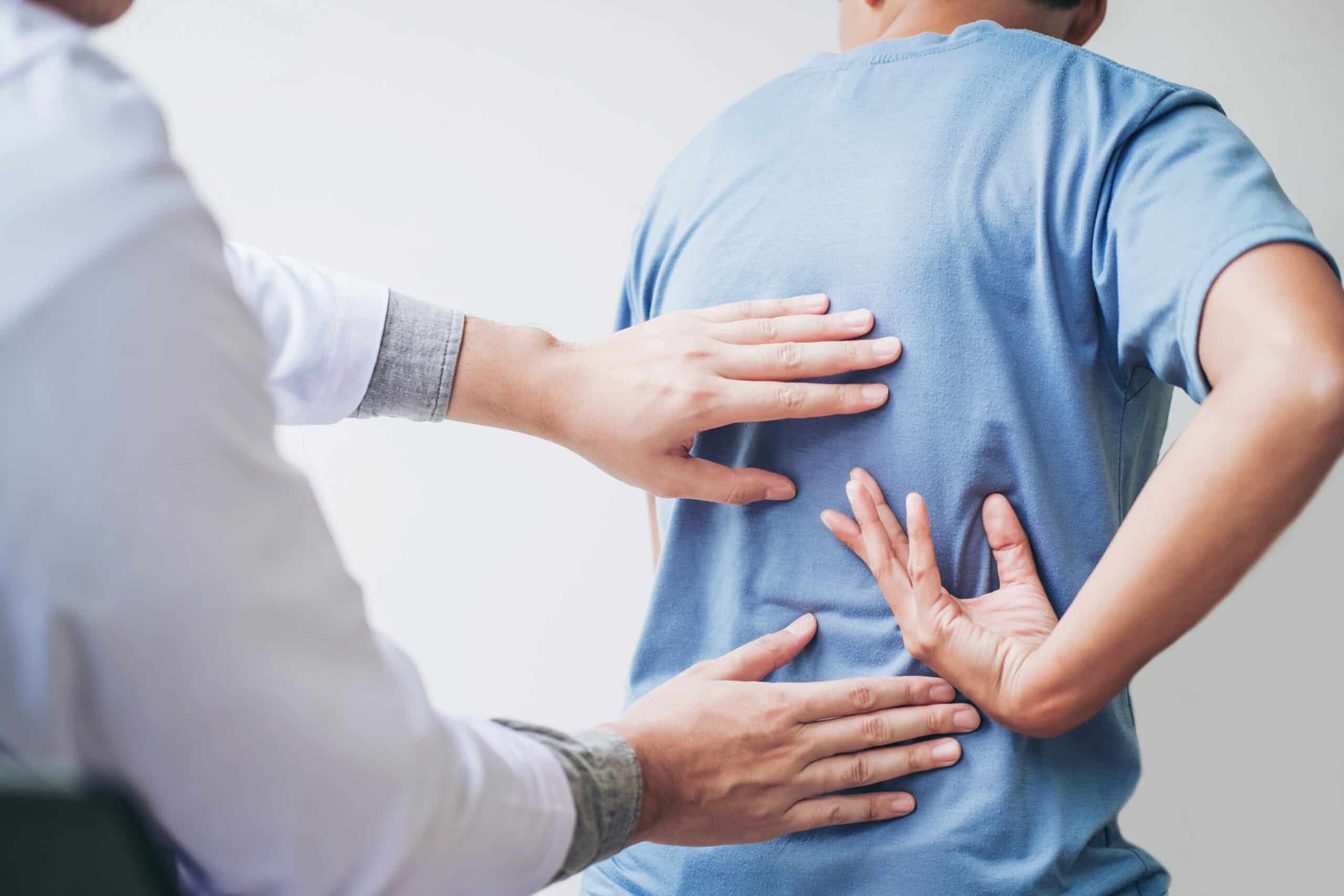
A trusted partner in spine care since 1992. As an independent medical center at the forefront of advanced spine restoration, our patients come to us seeking help. Whether they’re grappling with pain, unable to work, seeking second opinions, or pursuing solutions following unsuccessful treatments elsewhere, their common goal is clear—they want to reclaim their lives and we are here to provide solutions.
We’re Different
We believe patients deserve only the best.
We’re Independent
Providing you the care that you deserve: personalized treatment tailored to meet your unique needs.
We’re Visionary
Driven to continually advance solutions and technologies to benefit you: our patients.
We’re Collaborative
Defined by the power of us – our team, colleagues, and patients – working together to achieve Victories.
Our Patients’ Victories
Everything we do, we do for our patients – providing them with solutions that help them get their lives back.
Living Life Again
At VSI, we celebrate every patient’s unique journey as a series of victories, regardless of how big or small. Our logo and brand were crafted for you, our incredible patients. Your progress towards your goals deserves the spotlight, reflecting our commitment to individualized treatment and care. Your Victories are what make VSI who we are! #MyVictoryStory
Our Solutions
With a comprehensive suite of services, we provide a full range of customized solutions not found elsewhere.
Featured Resources
Insights to Achieve a Pain-Free Life