Pseudarthrosis
UNDERSTANDING THE SYMPTOMS, CAUSES AND TREATMENTS
Understanding Pseudarthrosis
Pseudarthrosis or nonunion is the failure of complete spinal fusion and healing. Often, patients report resolution of their symptoms right after their spinal surgery. Unfortunately, several months after their fusion, patients typically experience a return of their axial neck or back pain. Pseudarthrosis can be evaluated on x-rays as either lucencies around the implants and hardware or as motion at the “fused” level. Typically, your surgeon will also order a CT scan of the affected area to confirm whether or not the fusion completely healed. Treatment options vary from non-surgical to surgical care.
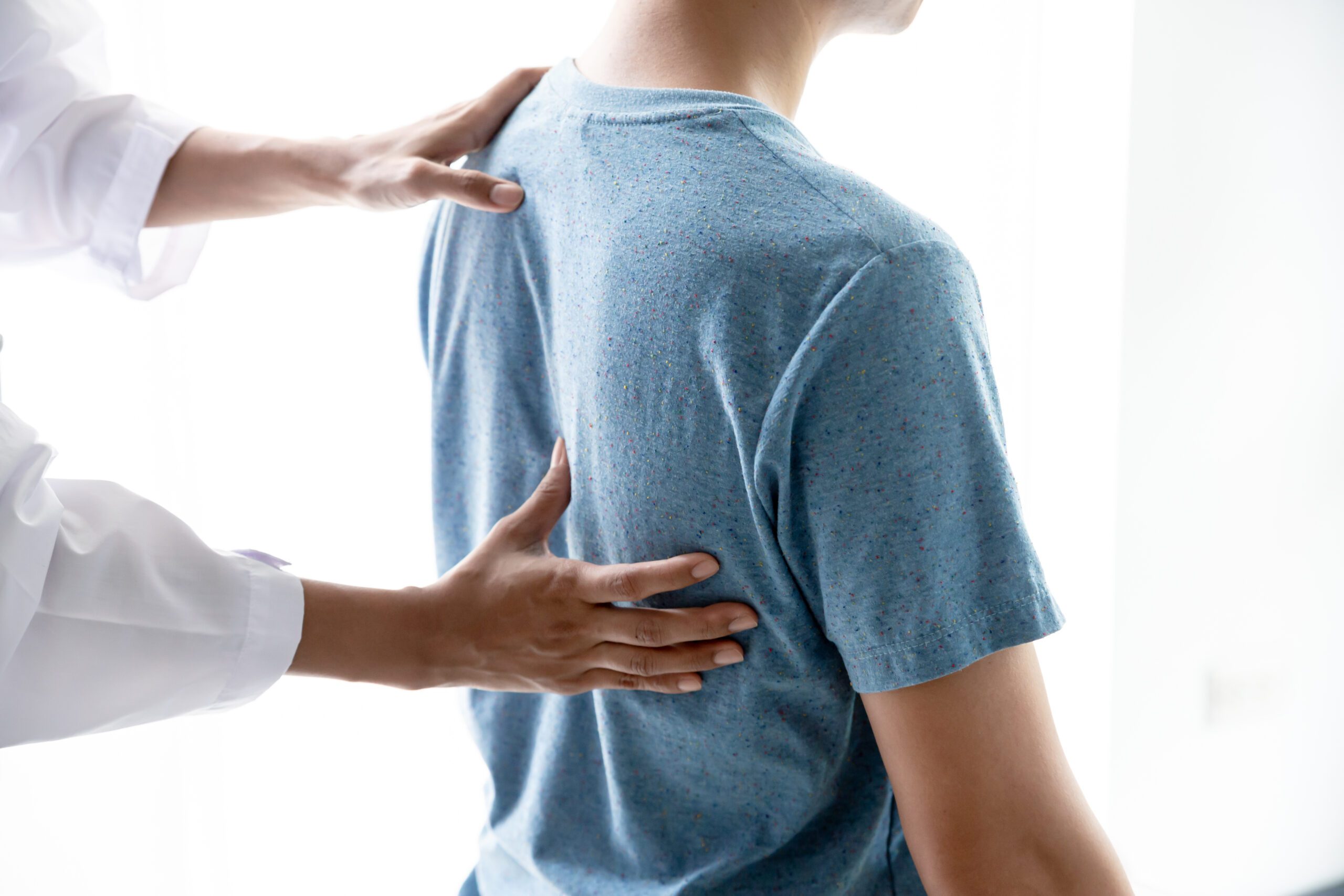
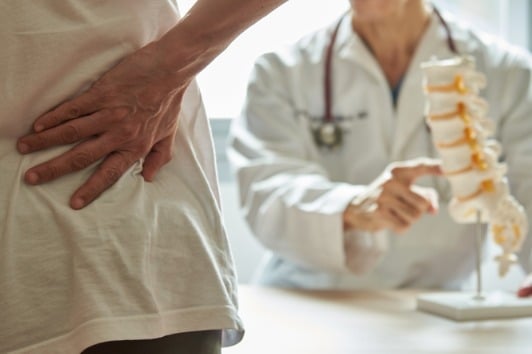
Symptoms
After undergoing any fusion surgery patients have three months of postsurgical restrictions. During the initial postsurgical period often patients feel significant relief of their pre-surgical pain but have the expected surgical and incision discomfort. Once patients are beyond their postsurgical restriction period and they return to normal activities there is often some return of pain as they are deconditioned. However, several months after surgery if the patient reports return of pre-surgical pain, worsening pain, or neurologic symptoms such as numbness or tingling pseudarthrosis is often the culprit. Often pain is described as an axial neck or back pain which is pain that radiates to the sides of your neck or back. Patients are at higher risk of a non-union if they have a history of previous pseudarthrosis, history of diabetes, or multiple levels treated at once.
When to Seek Treatment
If you’re noticing symptoms associated with Pseudarthrosis and suspect a spinal issue, it’s crucial to consider consulting a board-certified spinal specialist. Reach out promptly to a certified spine surgeon for an accurate diagnosis and timely treatment. Early intervention can significantly improve your overall well-being and provide a broader range of treatment options, which may decrease as symptoms persist. The key to a successful and speedy recovery lies in addressing the root of the pain with your spine specialist as soon as symptoms arise.
While many people experience day-to-day back or neck pain, dismissing it as soreness, this may not be the case for everyone. If your pain persists for more than 10 days, it should be taken more seriously. Evaluate such prolonged pain with a spine surgeon to identify the root issue and determine the appropriate treatment. Additionally, be attentive to other signs related to back or neck pain that should not be ignored, including pain accompanied by fever, pain associated with loss of bladder control, and weakness/tingling/numbness in your arms or legs.
It’s important to note that these are general guidelines based on our expertise in spine care over the past three decades, recognizing that each patient’s symptoms may be unique.

Common Causes
One of the goals of fusion surgery is for the bones to heal together or “weld” into one solid piece of bone. For fusion surgeries, bone graft is used to achieve fusion and the fusion heals much in the same way a broken bone heals in a cast. If the bones do not “weld together” properly, then motion may continue across the area. For some patients, motion in that area can cause pain similar to that of a broken bone that never heals. Many patients with pseudarthrosis have no symptoms. For these asymptomatic patients, often further treatment or evaluation is not necessary as the risk of revision surgery outweighs the benefit. However, for those symptomatic patients, x-rays and CT scans of the spine may be used to determine if a spinal fusion has occurred.
Diagnosing Pseudarthrosis
When patients present to our office having had previous spinal surgery, we not only take a thorough medical history but also review any previous imaging and/or update imaging studies. The goal of any surgery is to treat symptoms and return patients to a good quality of life. If patients report they did well for a few months after surgery then symptoms return, often in the same distribution as their pre-surgical pain, we are suspicious of pseudarthrosis.T o confirm a non-union or pseudarthrosis imaging is required. During office visits we obtain x-ray imaging to fully evaluate your spine. These images typically include standing AP, lateral, flexion and extension views. Bones on an x-ray appear dense whereas discs often appear black like an empty space between vertebral bodies. A spinal fusion removes the disc and bone will form between two separate vertebral bodies making them one larger unit. If a pseudarthrosis is present typically there is a lucency, or darkness, where there should be bone. Also on standing flexion and extension radiographs motion may be seen which is abnormal in a well-healed fusion. A computed tomography (CT) scan is a more advanced imaging system to evaluate bony anatomy. CT scans are often used to confirm pseudarthrosis.
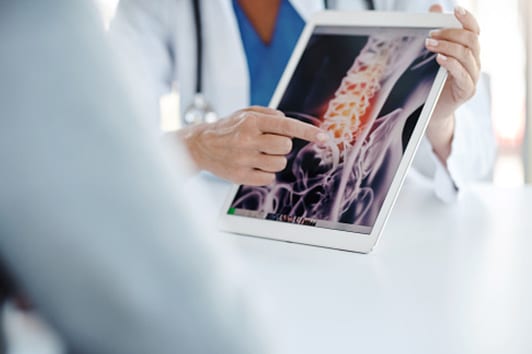
Treatment Options
Treatment of the patient with symptomatic pseudarthrosis involves a second attempt at fusion. Recent surgical advances including the use of spinal instrumentation, bone graft substitutes, and genetic engineering (bone morphogenetic protein) have helped surgeons decrease the risk of pseudarthrosis after spine fusion surgery.
Non-surgical treatments include physical therapy, anti-inflammatory medications, injections and physical therapy.

