Spondylosis
UNDERSTANDING THE SYMPTOMS, CAUSES AND TREATMENTS
Understanding Spondylosis
Our bodies change as we get older, and this can have a significant impact on our overall health –including the health of our neck and back. Referred to sometimes as arthritis of the spine, spondylosis is part of the aging process. Over time everyone will have this condition, however, symptoms are variable and are not dependent on how “bad” pictures can look. Seeing a lot of arthritis on the X-ray does not correlate with increased symptoms.
The spine is made up of a small system of bones called vertebrae. These vertebrae are separated by discs. These discs prevent the vertebrae from rubbing against each other, and they prevent the bones from pinching the nerves. As these discs begin to wear down, people will start to develop arthritis in the spine. Where it becomes a problem is when concerning symptoms become present, and could cause progressive neurological damage.


Symptoms
Similar to other conditions, symptoms can vary significantly depending on the scope and severity of the condition. Some of the most common symptoms include:
- Back or neck pain
- Radiating pain traveling to the arms or shoulders
- A feeling of weakness, numbness, or tingling in the arms or legs
- Muscle stiffness, spasms, or pain
- Difficulty with balance
- Bowel or bladder incontinence
- Difficulty with fine motor skills
Anyone who develops these symptoms needs to reach out to a doctor as soon as possible for treatment. Early diagnosis is key to preventing permanent neurological damage.
When to Seek Treatment
If you’re noticing symptoms associated with Spondylosis and suspect a spinal issue, it’s crucial to consider consulting a board-certified spinal specialist. Reach out promptly to a certified spine surgeon for an accurate diagnosis and timely treatment. Early intervention can significantly improve your overall well-being and provide a broader range of treatment options, which may decrease as symptoms persist. The key to a successful and speedy recovery lies in addressing the root of the pain with your spine specialist as soon as symptoms arise.
While many people experience day-to-day back or neck pain, dismissing it as soreness, this may not be the case for everyone. If your pain persists for more than 10 days, it should be taken more seriously. Evaluate such prolonged pain with a spine surgeon to identify the root issue and determine the appropriate treatment. Additionally, be attentive to other signs related to back or neck pain that should not be ignored, including pain accompanied by fever, pain associated with loss of bladder control, and weakness/tingling/numbness in your arms or legs.
It’s important to note that these are general guidelines based on our expertise in spine care over the past three decades, recognizing that each patient’s symptoms may be unique.

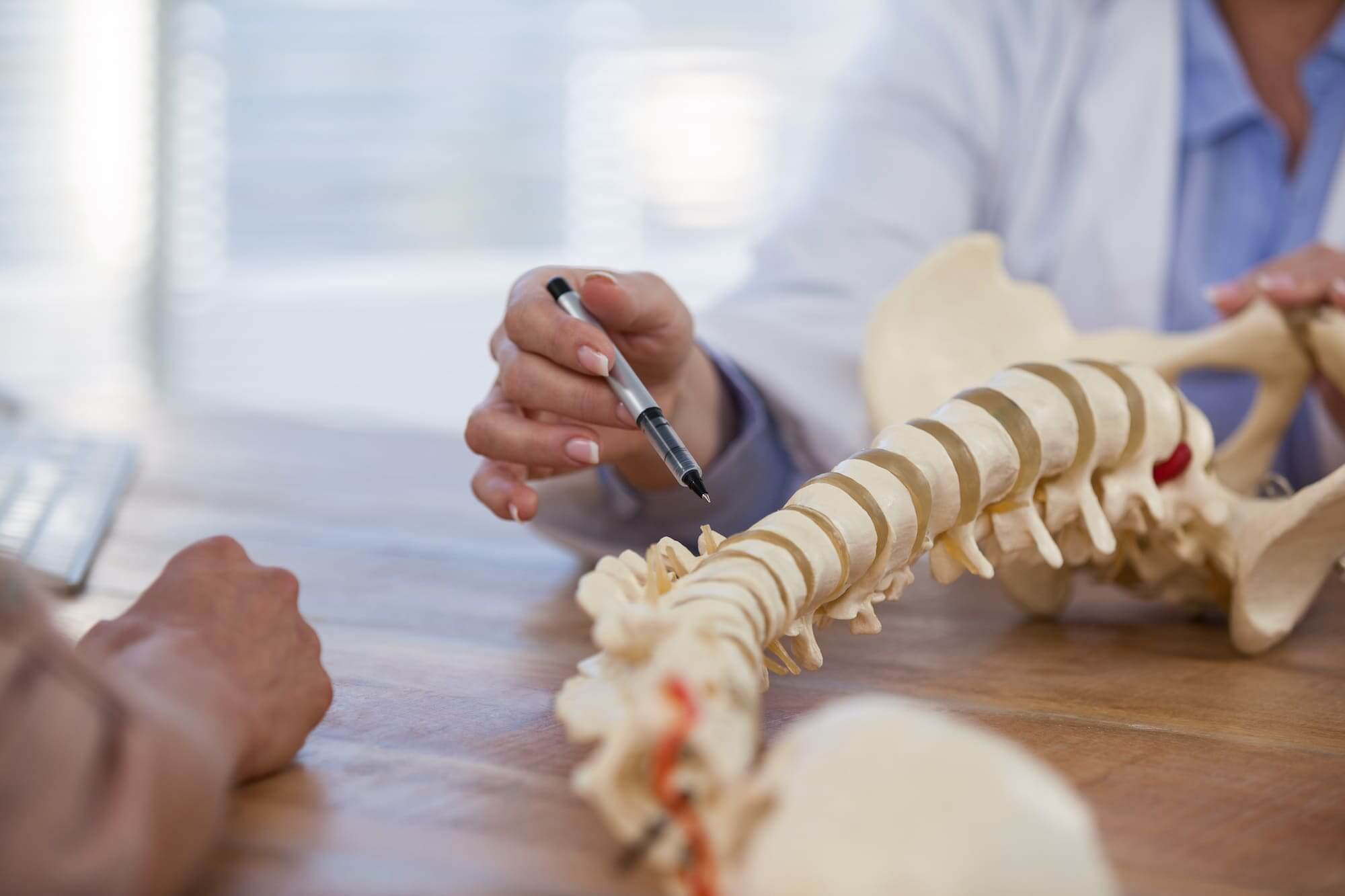
Common Causes
There are several possible reasons why someone may develop spondylosis, including:
- Herniated Discs: If someone has a history of one or more herniated discs, they are at risk of developing arthritis in the spine. A herniated disc develops when one of the disks in the spine ruptures. This can cause the vertebrae to rub against each other, leading to inflammation and arthritis.
- Degenerative Discs: Someone can also be diagnosed with degenerative discs. The discs are filled with fluid that creates a cushion between the vertebrae. When the discs degenerate, the vertebrae can rub against each other, leading to arthritis.
- Bone Spurs: Bone spurs can also lead to the development of this condition. Bone spurs can cause inflammation, causing them to rub against different portions of the spine. This can lead to arthritis.
Risk Factors
There are several risk factors that could make it more likely for someone to develop arthritis of the spine. They include:
- Someone who is older has a greater chance of developing arthritis of the spine when compared to someone who was younger
- Individuals who work in a job that involves repeated neck motion
- Someone with a prior history of neck injuries
- People who smoke
- Someone with a lot of relatives who have been diagnosed with spondylosis is at a greater risk of developing this condition themselves
There are numerous other risk factors that could make it more likely for someone to develop this condition, and these are just a few of the most common examples.

Diagnosing Spondylosis
There are several steps involved in the diagnosis of spondylosis. During the initial consultation with your doctor, a detailed medical history as well as comprehensive physical exam is completed to better understand your specific time-line and triggers of pain.
Once the exam has been completed, your doctor could order imaging scans to take a closer look at the vertebrae and spinal discs. Imaging is key for the proper diagnosis of spondylosis often including x-rays taken of the affected area. And if further evaluation is needed, CT and MRI scans may be ordered
Treatment Options
There are several treatment options that could be tried. Some of the most common treatment options include:
- Physical Therapy: Physical therapy can be used to strengthen muscles, ligaments, and tendons. This will provide additional support to the spine, alleviating some of the symptoms of the condition.
- Medications: Medications are also frequently used to manage the symptoms of arthritis. Over-the-counter anti-inflammatory medications could be recommended, and patients may also be given steroid injections to further reduce inflammation.
- Surgery: In certain cases, surgical intervention may be recommended depending on the patient’s severity of symptoms or the presence of progressive neurologic damage.
The treatment plan is tailored to meet the needs of the individual. Not everyone who is diagnosed with spondylosis will require surgery.


Prevention
There are a few ways that individuals can prevent arthritis from developing in the spine. Some of the most important preventative techniques that people need to know include:
- Avoid High-Impact Exercise: People who perform high-impact exercise are at a greater risk of developing the condition. What this means is that if there is a lot of pounding on the feet and knees, this can be transferred to the spine, leading to arthritis.
- Maintain Neck Range of Motion: People also need to maintain a solid range of motion in the neck. There are exercises that people can perform that can increase the range of motion in the neck, reducing the chances of developing arthritis. For example, even rotating the head from side to side a few times a day can improve the range of motion.
- Avoid Smoking: People also need to make sure they avoid smoking. Smoking is one of the most important risk factors for the development of spondylosis, and people who avoid smoking will be at a lower risk of developing this condition.
These simple changes can reduce someone’s chances of developing arthritis of the spine.

