Non-Surgical Solutions
What Are
Non-Surgical Solutions?
We know not everyone is a candidate for surgery and were founded on the principle of providing non-surgical solutions to our patients. We’re proud to offer an extensive range of cutting-edge non-surgical treatments. These include regenerative medicine, spine-specialized physical therapy, acupuncture, and an array of injections and diagnostic testing through our team of specialists.

Spine-Specialized
Physical Therapy
At VSI Physical Therapy, our total wellness model treats beyond pain relief and promotes long-term wellness benefits. In our state-of-the-art facility, patients can experience hands-on manual therapy, aquatic therapy, therapeutic massage, nutrition coaching, rehabilitative personal training, and fitness instruction. With over 20 years of patient care, we’ve grown to one of the most dynamic physical therapy practices in the area — offering solutions that are not offered anywhere else.
Natural Healing
With Physical Therapy
Regenerative medicine is a modern non-operative treatment solution that utilizes the body’s natural healing process to rebuild damaged tissue, heal injuries more effectively, and eliminate pain. Regenerative medicine targets the underlying source of pain without relying on medication or surgery and leads to increased function and mobility with a shorter recovery time than surgical options.
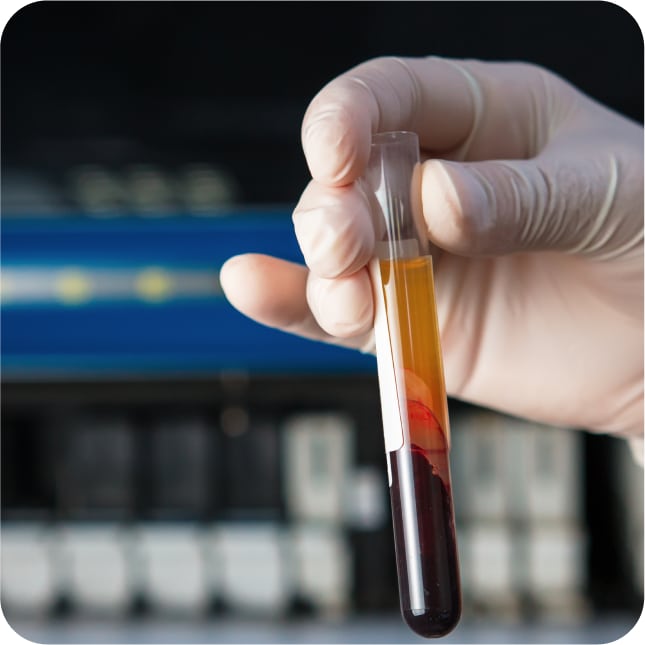
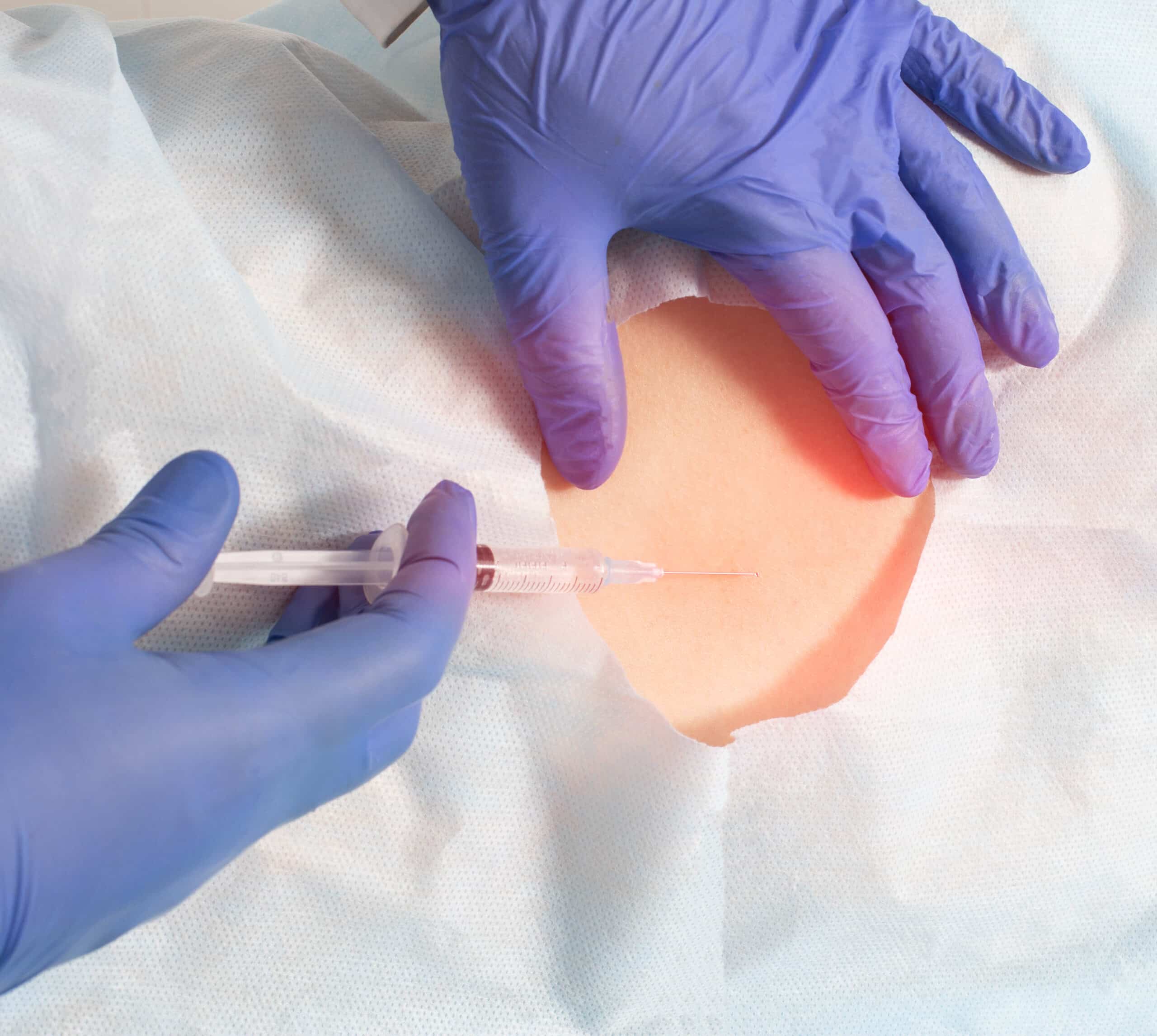
Non-Operative
Injections
Injections of medications to decrease pain and inflammation have long been used in pain medicine as additional, adjunctive treatment to medications. Traditionally, it has always been a combination of a steroid and a local anesthetic agent. The steroid acts to interrupt the inflammatory cascade that leads to pain and swelling. The local anesthetic provides immediate pain relief to provide diagnostic confirmation of the pain generator as well as to break the pain cycle in certain chronic pain syndromes like Complex Regional Pain Syndrome (CRPS) and trigger points.

Acupuncture
In the United States, acupuncture has found its greatest acceptance and benefit in the treatment and management of musculoskeletal pain. Acute musculoskeletal and myofascial conditions such as sprains, strains, spasms and contusions are among the problems most frequently and successfully treated to resolution with acupuncture. In such cases, acupuncture can be legitimately considered as a first line treatment.

