Spinal Stenosis
UNDERSTANDING THE SYMPTOMS, CAUSES AND TREATMENTS
Understanding Spinal Stenosis
Without treatment, spinal stenosis can significantly impact your mobility and quality of life.
The spinal cord is a long, tubular structure that connects the brain to the peripheral nervous system, allowing you to move your body, feel your surroundings, and experience pain.
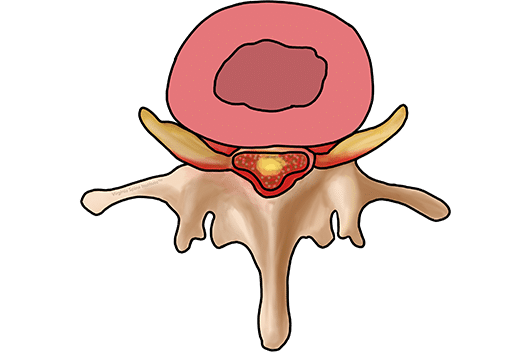
The spinal column protects our spinal cord and is made up of bones, joints, discs, soft tissues, and nerves. The spinal cord is housed in the cervical and thoracic spine and normally terminates at the upper lumbar spine, where the nerves then spread out and travel freely through the canal. Think about the spinal cord and nerves as a spaghetti noodle traveling through a straw. Think about spinal stenosis as the straw getting smaller and smaller, providing little room for the spaghetti noodle to fit.
Cervical spinal stenosis causes pressure on the spinal cord and exiting spinal nerves. Lumbar spinal stenosis causes pressure on the freely traveling and exiting lumbar spinal nerves. This can be caused by several factors including degenerative changes such as disc herniations, disc height collapse, enlargement of facet joints, arthritis, or thickening of the ligamentous structures.
Spinal stenosis is diagnosed when medical imaging demonstrates narrowing of the spinal canal or foramen where the spinal nerves exit.

Symptoms
Symptoms depend on the location, and whether it affects the spinal cord or spinal nerves.
If the spinal cord is compressed in the cervical or thoracic spine, you may or may not experience pain or symptoms of radiculopathy. Often, spinal cord stenosis presents with symptoms of myelopathy. Myelopathy is a term used to describe neurologic symptoms related to the spinal cord that may cause permanent spinal cord injury. Without spinal stenosis treatment, damage may lead to paralysis or death. Symptoms of myelopathy include:
- Balance difficulty
- Heaviness in the arms or legs
- Abnormal gait
- Dropping objects
- Clumsiness or difficulty with fine motor skills, such as typing or writing
If only the spinal nerve roots are involved, you may experience pain, numbness, tingling, or weakness in the arms or legs, called radiculopathy.
Lumbar spinal stenosis may cause pain and radiculopathy or symptoms of neurogenic claudication. Symptoms of neurogenic claudication include pain, numbness, weakness, tingling, or heaviness in the legs that often worsen with prolonged standing or walking.
Pain often is improved with sitting or bending forward. If lumbar spinal stenosis is severe enough, it can result in cauda equina syndrome. That is when the bundle of nerves below the spinal cord is compromised, causing loss of sensation in the genital area, bowel or bladder incontinence, urinary urgency, leg pain or weakness, numbness, or heaviness in the legs.
Cauda equina syndrome is a spinal emergency and requires emergent evaluation as it can lead to permanent paralysis and incontinence.
When to Seek Treatment
If you’re noticing symptoms associated with Spinal Stenosis and suspect a spinal issue, it’s crucial to consider consulting a board-certified spinal specialist. Reach out promptly to a certified spine surgeon for an accurate diagnosis and timely treatment. Early intervention can significantly improve your overall well-being and provide a broader range of treatment options, which may decrease as symptoms persist. The key to a successful and speedy recovery lies in addressing the root of the pain with your spine specialist as soon as symptoms arise.
While many people experience day-to-day back or neck pain, dismissing it as soreness, this may not be the case for everyone. If your pain persists for more than 10 days, it should be taken more seriously. Evaluate such prolonged pain with a spine surgeon to identify the root issue and determine the appropriate treatment. Additionally, be attentive to other signs related to back or neck pain that should not be ignored, including pain accompanied by fever, pain associated with loss of bladder control, and weakness/tingling/numbness in your arms or legs.
It’s important to note that these are general guidelines based on our expertise in spine care over the past three decades, recognizing that each patient’s symptoms may be unique.

Common Causes
Spinal stenosis is a narrowing of the spinal canal to a degree where the spinal cord or nerve roots become compromised. Spinal stenosis may occur in any area of the spine, but it is most common in the lumbar spine. However, spinal stenosis is most dangerous in the cervical and thoracic spine due to its proximity to the spinal cord.
There are several causes of spinal stenosis; however, degenerative changes are typically the most common. These changes include:
- Disc height collapse
- Disc herniations
- Thickening of ligaments
- Arthritic changes
- Tumors
Finally, bone spur formation, called spondylosis, is also a common cause.
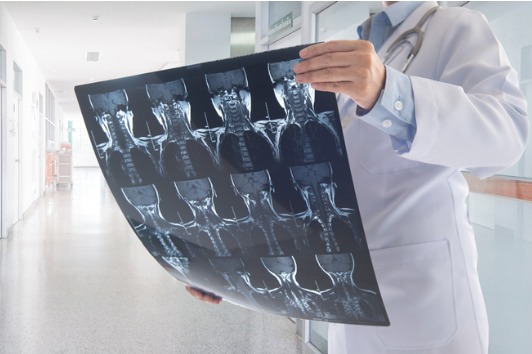
Diagnosing Spinal Stenosis
There are several steps involved in the diagnosis of spinal stenosis. During the initial consultation with your doctor, a detailed medical history as well as comprehensive physical exam is completed to better understand your specific time-line and triggers of pain.
Once the exam has been completed, your doctor could order imaging scans to take a closer look at the vertebrae and spinal discs. Imaging is key for the proper diagnosis of spinal stenosis, often including x-rays taken of the affected area. And if further evaluation is needed, CT and MRI scans may be ordered.
Treatment Options
For people with mild spinal stenosis and not at risk for permanent neurologic deficit, conservative treatments often are the initial treatment of choice. These non-surgical treatments include spine specialized physical therapy in conjunction with medications.
Physical therapy gently stretches the joints and muscles in the spine to provide relief. PT should also help you develop an effective home exercise program to build your core and cardiovascular endurance. Chiropractic manipulation should never be performed with spinal stenosis. When medications and therapy fail to improve symptoms, steroid injections may be recommended to reduce inflammation. However, if your symptoms progress despite the above remedies or if you develop neurologic symptoms/deficit, then it is important to discuss surgical options.
The goal of spinal stenosis treatment with surgery is to improve pain and stop progressive neurologic damage.
Multiple surgical procedures and approaches exist to treat spinal stenosis. Our spinal specialists at the VSI will review these options with you. Each surgical plan is specifically tailored to the patient and their spinal needs to provide the best care possible and optimal recovery.



