Spondylolisthesis
Understanding the Symptoms, Causes & Treatments of Spondylolisthesis
Reviewed by: Dr. Christopher Good, Dr. Colin Haines, Dr. Ehsan Jazini
What is Spondylolisthesis?
Spondylolisthesis is a medical diagnosis to describe the forward slippage of one vertebral body in relation to the vertebra below. The spine is made of several motion segments stacked on top of one another to allow for smooth movement in all directions. Each of these segments has three major points of contact including two facet joints and an intervertebral disc. If the facet joint and intervertebral discs degenerate or experience trauma this could lead to abnormal motion and misalignment. Another common cause of spondylolisthesis often diagnosed and treated by the specialists at VSI is a stress fracture in the vertebra.
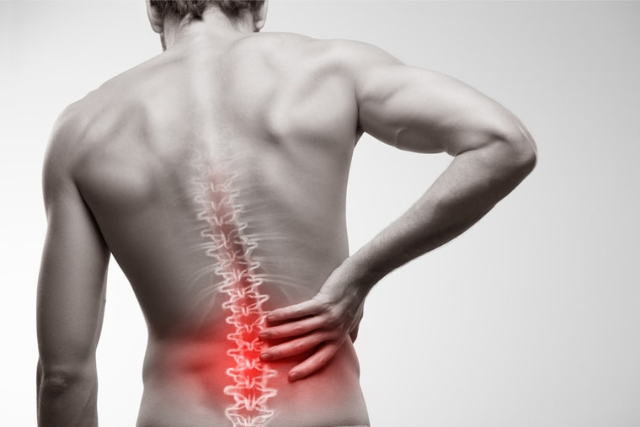
What Are Common Symptoms of Spondylolisthesis?
Symptoms of spondylolisthesis depend on the severity of slippage. Symptoms can include pain, discomfort, stiffness, or muscle spasms in the low back. Symptoms of radiculopathy may appear including numbness, tingling, pain, or weakness in the legs. If the slippage is severe and causes detrimental pressure on the spinal nerves, you may develop symptoms of cauda equina syndrome. These include numbness in the groin area or down the legs, loss of bowel or bladder control, urinary urgency, or difficulty with balance or walking. Cauda equina is a spinal emergency and if you are experiencing these symptoms seek immediate evaluation.
When to Seek Treatment for Spondylolisthesis?
If you’re noticing symptoms associated with Spondylolisthesis and suspect a spinal issue, it’s crucial to consider consulting a board-certified spinal specialist. Reach out promptly to a certified spine surgeon for an accurate diagnosis and timely treatment. Early intervention can significantly improve your overall well-being and provide a broader range of treatment options, which may decrease as symptoms persist. The key to a successful and speedy recovery lies in addressing the root of the pain with your spine specialist as soon as symptoms arise.
While many people experience day-to-day back or neck pain, dismissing it as soreness, this may not be the case for everyone. If your pain persists for more than 10 days, it should be taken more seriously. Evaluate such prolonged pain with a spine surgeon to identify the root issue and determine the appropriate treatment. Additionally, be attentive to other signs related to back or neck pain that should not be ignored, including pain accompanied by fever, pain associated with loss of bladder control, and weakness/tingling/numbness in your arms or legs.
It’s important to note that these are general guidelines based on our expertise in spine care over the past three decades, recognizing that each patient’s symptoms may be unique.

What Are Common Causes of Spondylolisthesis?
The spine is made up of bones, discs, soft tissues, and nerves. There are 7 cervical, 12 thoracic, and 5 lumbar vertebral bodies to make up the spinal column. Each of these vertebral bodies is stacked one on top of another. Between the vertebral bodies are intervertebral discs which act as the shock absorbers of the spine which naturally degenerate as we age. There are two different types of spondylolisthesis: degenerative and isthmic.
A pars fracture also known as spondylolysis is a fracture of the pars interarticularis. Isthmic spondylolisthesis is the medical term for slippage due to this type of fracture. In non-medical terms, this means the fracture caused instability, and over time the vertebral body slipped forward. This type of fracture may be the result of direct trauma or from a genetic weakness in this area of the bone and commonly occurs in adolescence.
Degenerative spondylolisthesis is caused by arthritic changes to the facet joints or degeneration of the intervertebral disc. With degenerative disc disease, intervertebral discs progressively break down. The discs lose hydration, there’s a decrease in disc height and function. They are no longer able to provide good structural stability. Recall facet joints are part of the three-joint complex stabilizing the spine. As the facet joints degenerate small ligaments supporting the joint wear down and loosen. This laxity allows the joint to separate more often contributing to a slippage or spondylolisthesis.
How is Spondylolisthesis Diagnosed?
To properly diagnose a spondylolisthesis, weight-bearing x-rays are required. Typical imaging studies include AP, lateral, flexion, and extension lumbar views. These vital imaging studies allow your spinal specialists not only to diagnose a spondylolisthesis but also to grade the severity of this slippage. There are 5 different grades of spondylolisthesis and the higher the grade the increased risk of neurologic symptoms.
What Are Common Treatments for Spondylolisthesis?
There are many different treatment options for spondylolisthesis depending on the severity of the patient’s symptoms and the degree of slippage. Often, non-operative treatments are started initially. These include spine-specialized physical therapy, core strengthening, manual massage, dry needling, low-impact exercise, and maintaining an overall healthy lifestyle.
If patients fail non-operative treatment or are developing worsening neurologic symptoms, surgery is often discussed. There are many different approaches for surgical intervention which your spinal specialist at VSI will discuss with you in detail. The goal of surgical intervention is to stabilize the spine, alleviate pressure from the nerves, and correct any structural deformity. Every surgical plan is personalized to our patients depending on his or her symptoms or spinal needs.

