Bone Spurs
Understanding the Symptoms, Causes & Treatments for Bone Spurs
Reviewed by: Dr. Christopher Good, Dr. Colin Haines, Dr. Ehsan Jazini
What are Bone Spurs?
Many patients are told that they have bone spurs or osteophytes in their back or neck. Bone spurs are simply an indication that there are increased forces on the joints of the spine. With increased forces on the intervertebral discs and facet joints in the spine, instability may occur as well. In response to this over time, the body remodels bone to decrease the stress on the joints or to increase surface area to prevent instability.
In many cases, osteophytes and other degenerative changes may be considered the normal process of aging. Their presence does not necessarily mean that they are the actual cause of pain. However, there are a number of common spinal conditions associated with pain that are related to their development. These conditions include spondylosis, cervical or lumbar radiculopathy, and spinal stenosis.


What are Common Symptoms of Bone Spurs?
Patients with osteophytes that are symptomatic often describe stiffness in the neck, mid or lower back. This stiffness may be associated with a dull ache and possibly a lack of mobility or range of motion. This lack of mobility is often noted in the neck and lower back when patients attempt to bend forwards or backward or rotate left or right. The presence of bone spurs may be an indication of an underlying spinal condition, for example, degenerative disc disease. Depending on the extent and location of the bone spur, the nerves branching off of the spinal cord may be affected. If this is the case, patients may also experience radicular symptoms such as pain, numbness, or tingling that radiates into the arms or legs.
When Should You Seek Treatment for Bone Spurs?
If you’re noticing symptoms associated with Bone Spurs and suspect a spinal issue, it’s crucial to consider consulting a board-certified spinal specialist. Reach out promptly to a certified spine surgeon for an accurate diagnosis and timely treatment. Early intervention can significantly improve your overall well-being and provide a broader range of treatment options, which may decrease as symptoms persist. The key to a successful and speedy recovery lies in addressing the root of the pain with your spine specialist as soon as symptoms arise.
While many people experience day-to-day back or neck pain, dismissing it as soreness, this may not be the case for everyone. If your pain persists for more than 10 days, it should be taken more seriously. Evaluate such prolonged pain with a spine surgeon to identify the root issue and determine the appropriate treatment. Additionally, be attentive to other signs related to back or neck pain that should not be ignored, including pain accompanied by fever, pain associated with loss of bladder control, and weakness/tingling/numbness in your arms or legs.
It’s important to note that these are general guidelines based on our expertise in spine care over the past three decades, recognizing that each patient’s symptoms may be unique.

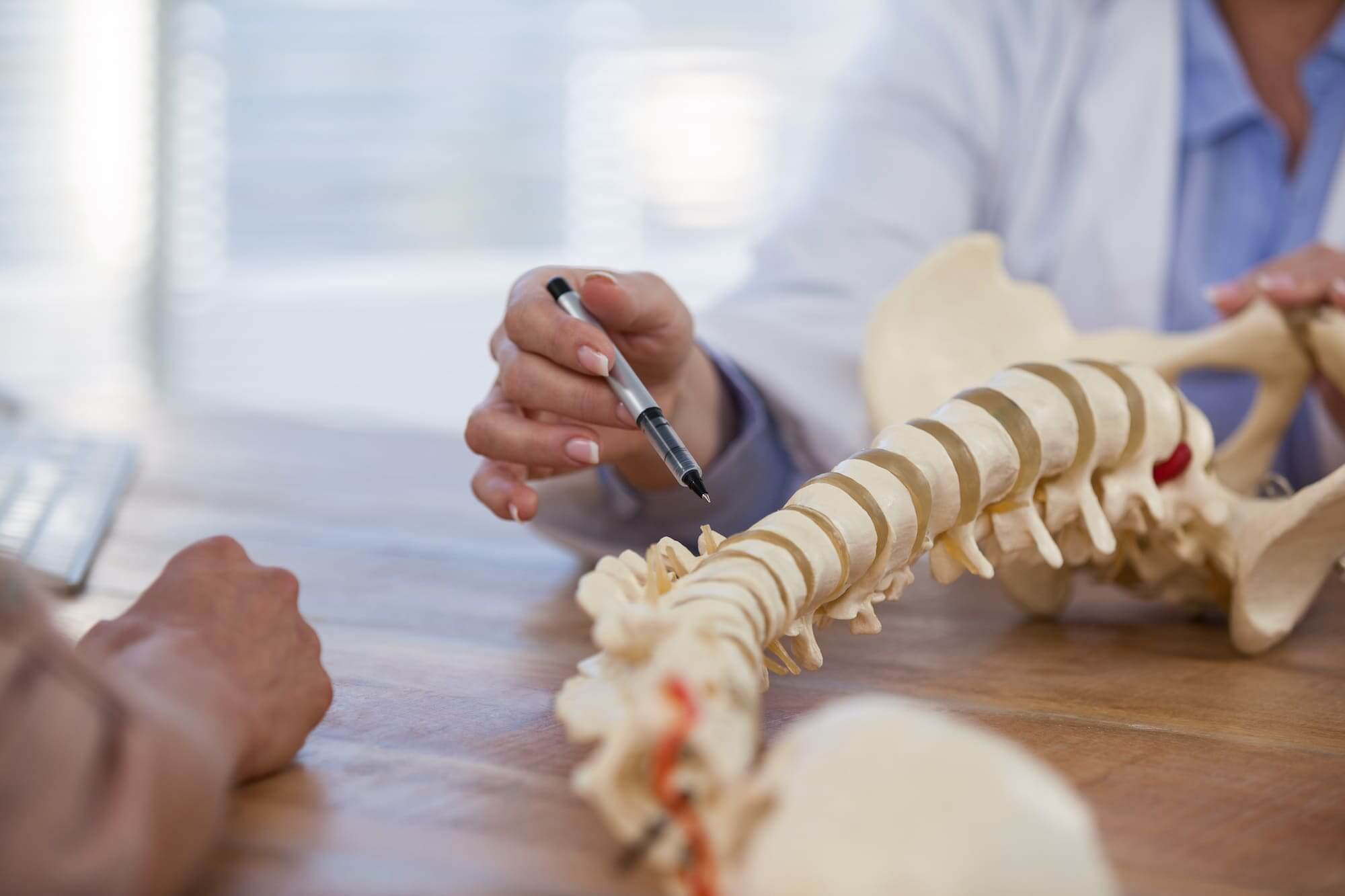
What are Common Causes of Bone Spurs?
Typically osteophytes are caused by degeneration in the joints of the spine as well as part of the natural aging process. In some cases, trauma, injury, and osteoarthritis can cause bone spurs.
Who is at Higher Risk for Bone Spurs?
There are several risk factors that could make it more likely for you to develop bone spurs or osteophytes. Some of these risk factors include:
- Aging
- Obesity – Excess weight may produce increased force across a joint, especially in a weight-bearing joint, that may lead to arthritis or spondylosis which typically cause osteophytes
- Joint Injury – Arthritis, which may lead to osteophytes, may develop after an injury to a joint involving ligament tears or fractures.
- Genetics – There are heredity forms of arthritis due to certain rare mutations in structural collagen types found in articular cartilage.

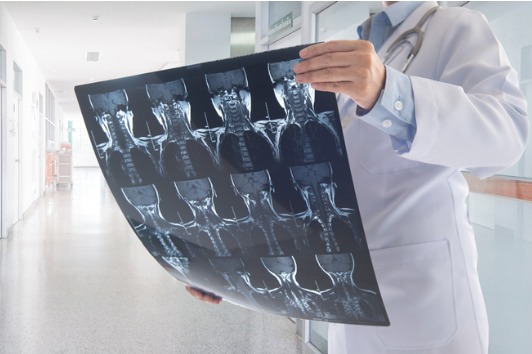
How are Bone Spurs Diagnosed?
Bone spurs are often associated with other spinal conditions such as spondylosis or degenerative disc disease. Providers may be suspicious of these conditions if abnormal range of motion is noted on a physical exam. Diagnosis of osteophytes can be made easily with x-ray imaging. Standing radiographs of your neck, mid, or low back will be obtained depending on the location of your symptoms. In some instances, a further work-up is warranted and MRI or CT scans may be ordered.
What are Common Treatment Options for Bone Spurs?
Most patients with mild or moderate nerve compression from osteophytes can manage symptoms effectively with non-surgical care including:
- Rest
- Activity modification
- Spine-specialized physical therapy
- Medications
- Injection therapy
If these treatments do not alleviate symptoms, surgical intervention may be considered.


Can Bone Spurs be Prevented?
Understanding the root cause of your bone spur is the key to preventing further bone spurs. Sometimes, bone spurs are hereditary and underlying medical conditions can contribute to the formation of bone spurs. However, if it is caught early enough, conservative treatment options may be all you need in slowing down the growth of bone spurs and preventing new ones from forming.

