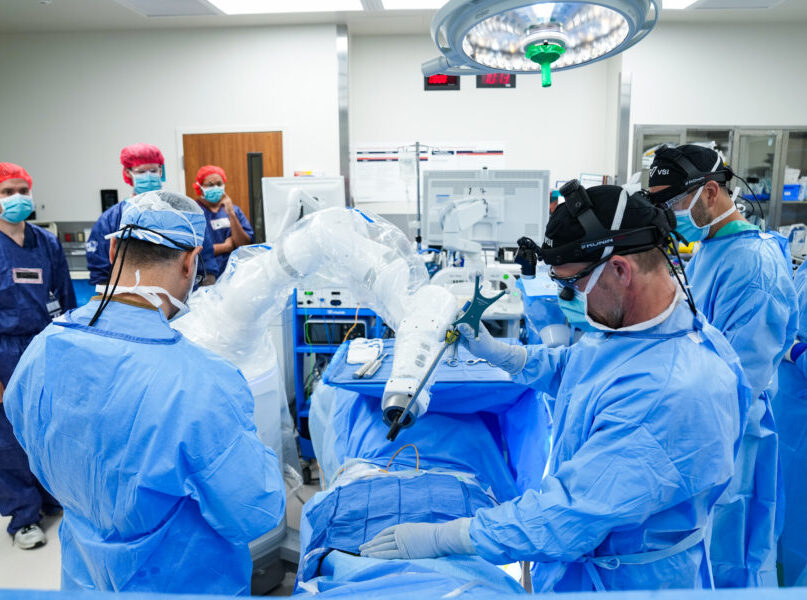
How to Reduce the Risks of Spine Surgery
Key Takeaways: Risks of Spine Surgery
- As with all surgery, spine surgery can carry risks, but those risks can often be reduced through accurate diagnosis, careful surgical planning, advanced technology, and a structured recovery plan.
- Most complications are uncommon and can often be prevented or effectively managed with proper planning and care
- Advances in surgical techniques and technology have improved safety, precision, and recovery outcomes
- At VSI, reducing surgical risk begins before surgery and continues through recovery. Each patient receives a personalized plan designed around their condition, health history, imaging, prior treatments, and long-term goals.
- Taking the right steps before and after surgery can significantly reduce risks and support a smoother recovery
Is Spinal Surgery Considered Safe?
Spine surgery is widely regarded as safe and effective, especially when it is recommended after conservative treatments have not provided sufficient relief. Advances in medical technology, imaging, and surgical techniques have made procedures more precise and less invasive, which has helped reduce complication rates and improve recovery times.
That said, no surgery is completely without risk. The safety of spine surgery depends on several factors, including the patient’s overall health and the experience of the surgical team. Minimally invasive procedures often involve smaller incisions and less disruption to surrounding tissue, which can lower the risk of complications and support a smoother recovery. More complex procedures, such as spinal reconstruction due to advanced scoliosis, may carry a higher risk but are still routinely performed with strong safety outcomes when carefully planned and performed by an experienced spine specialist.
For most patients, the decision to move forward with spine surgery comes down to weighing the potential risks against the expected benefits. When symptoms such as chronic pain, nerve compression, weakness, or loss of mobility significantly impact daily life, surgery can offer meaningful and lasting relief. With the right preparation and care team, patients can feel confident that every step is being taken to prioritize their safety, recovery, and long-term success.
What Are the Risks of Spinal Surgery?
Spine surgery risks vary based on the procedure, the patient’s health, and the complexity of the condition being treated. While all surgeries carry some level of risk, most complications associated with spine procedures are uncommon and often manageable when identified early.
Possible risks of spine surgery may include infection, bleeding, blood clots, nerve irritation or injury, anesthesia-related concerns, spinal fluid leaks, hardware complications, or symptoms that persist after surgery. In some cases, patients may need additional treatment if pain, numbness, weakness, or mobility limitations do not improve as expected.
Spine specialists evaluate each case individually to determine whether surgery is the right option. This includes reviewing: medical history, advanced imaging, prior treatments, symptoms, and recovery goals to ensure that the potential benefits outweigh the risks. With proper planning and a personalized approach, many risks can be reduced before surgery even begins.
When Prior Spine Surgery Did Not Fully Address Symptoms
Many patients come to VSI after a long and frustrating journey with spine pain. Some have already had surgery elsewhere, only to find that their symptoms were not fully addressed, their recovery was harder than expected, or complications affected their confidence in moving forward. For more, see Nick’s story below as he navigated the recovery with VSI after having a failed back surgery elsewhere.
At VSI, we understand that choosing spine surgery can feel overwhelming, especially when patients are carrying the weight of a previous experience. Persistent pain after surgery does not always mean that nothing can be done. It may mean the original pain generator needs to be re-evaluated, nerve compression needs to be reassessed, adjacent levels need to be reviewed, or the recovery plan needs a more comprehensive approach.
That is why VSI focuses on reducing risk at every stage of care, from diagnosis and surgical planning to advanced techniques, coordinated recovery, and long-term follow-up. The goal is not simply to perform spine surgery. The goal is to help each patient recover with greater confidence, clarity, and support.
What Factors Can Increase the Risk of Spinal Surgery?
The risks of spinal surgery are personal to each patient. Overall health, lifestyle, prior treatments, and the complexity of the condition being treated can all influence how the body responds to surgery and how smoothly recovery progresses. That is why understanding the full picture before surgery is so important.
At VSI, every surgical recommendation begins with a detailed evaluation, advanced imaging, and a conversation about each patient’s goals, health history, and recovery needs. This helps the care team identify concerns early, optimize the plan before surgery, and choose the safest, most effective approach for the individual patient. The goal is always to reduce avoidable risk while helping patients move forward with greater confidence.
How the Risks of Spine Surgery Can Be Minimized
While some level of risk is inherent in any surgical procedure, many of the risks associated with spine surgery can be reduced with the right preparation, surgical approach, and post-operative care. A proactive, personalized plan plays a key role in improving safety and outcomes.
Choosing an Experienced Spine Specialist
The skill and experience of the surgeon are among the most important factors in reducing surgical risk. Experienced spine specialists are better equipped to anticipate challenges, use precise techniques, and make informed decisions during surgery. Working with a qualified provider improves safety, reduces complication risk, and supports better long-term outcomes. Our team at VSI is board-certified and fellowship-trained, often called upon by other healthcare systems to educate and train their doctors in the surgical advancements we provide patients.

Ready to Take the Next Step?
Advanced Imaging, Testing and Surgical Planning
Advanced imaging and testing helps spine specialists better understand the source of pain, nerve compression, disc damage, instability, deformity, or prior surgical changes. Better visualization allows surgeons to operate with greater accuracy and avoid unnecessary disruption to surrounding tissue. Diagnostic testing, like EMGs, injections or discography, ensure your surgeon is operating on the correct level to relieve your symptoms. Careful planning reduces uncertainty during surgery and improves precision.
Using the Least Invasive Effective Approach
Not every patient needs the same type of spine surgery. When appropriate, minimally invasive techniques may reduce tissue disruption, blood loss, post-operative pain, and recovery time. The safest surgical plan is not always the smallest procedure; it is the procedure that best addresses the true source of symptoms while minimizing unnecessary risk.
Intraoperative Monitoring and Safety Protocols
Real-time monitoring of nerve function and vital signs during surgery allows the surgical team to detect potential issues immediately. Early detection and response can help reduce the risk of complications and protect neurological function.
Post-Surgical Care and Rehabilitation
Recovery plays a critical role in long-term success and complication prevention. Structured recovery plans, including follow-up care, movement guidance, and physical therapy, support healing and reduce the likelihood of setbacks.
What VSI Does to Help Reduce Surgical Risk
At VSI, reducing the risks of spine surgery starts long before the day of the procedure and continues throughout recovery. Every patient receives a personalized care plan built around their diagnosis, anatomy, health history, lifestyle, goals, and prior treatment experience.
For some patients, this means confirming whether surgery is truly necessary after conservative care has not provided relief. For others, it means re-evaluating symptoms after a previous spine surgery did not fully resolve their pain, mobility limitations, numbness, weakness, or nerve-related symptoms. In both cases, the priority is the same: identify the true source of the problem and create a plan that reduces avoidable risk while supporting the best possible outcome. Spine surgeon Dr. Colin Haines and physical therapist Larry Grine teamed up to dive deeper into collaborative recovery after major surgery and the importance of prehab and preparation for surgery.
Watch Recovery Resource on Youtube
VSI’s recovery-focused approach includes detailed pre-surgical evaluations, advanced imaging, thoughtful surgical planning, minimally invasive techniques when appropriate, intraoperative safety protocols, and coordinated post-operative care. This comprehensive model is designed to help patients move through surgery and recovery with greater precision, support, and confidence.
Recovery is not treated as an afterthought. It is a central part of the care plan. From follow-up visits to rehabilitation guidance, VSI helps patients understand what to expect, how to protect their progress, and when to ask for help. The goal is to reduce complications, support healing, restore function, and help patients get back to their lives with greater confidence.
When Is Spinal Surgery Necessary?
For many patients, spinal surgery becomes a consideration when symptoms begin to significantly impact daily life and non-surgical treatments are no longer effective.
Spinal surgery may be recommended when:
- Chronic pain limits normal activities or quality of life
- Nerve compression causes symptoms such as numbness, weakness, or loss of function
- Conservative treatments such as physical therapy, medication, or injections have not provided relief
In these situations, the potential benefits of surgery, including pain relief, improved mobility, and prevention of further damage, often outweigh the risks. A thorough evaluation with a spine specialist helps determine whether surgery is the right option based on each patient’s condition and goals.
Questions to Ask Your Spine Surgeon Before Surgery
Asking the right questions can help patients feel more informed and confident when considering spinal surgery.
Some helpful questions include:
- What are my specific risks based on my condition and health?
- Are there non-surgical options I should consider first?
- What is your experience with this type of procedure?
- What technology will be used during my surgery?
- Is there a more minimally invasive way to do this surgery?
- Is this recommended surgery my only option?
- What outcomes can I realistically expect?
- What will recovery look like, and how long will it take?
These conversations help ensure that patients understand both the benefits and risks, allowing them to make well-informed decisions.
Recovery & What to Expect After Spinal Surgery
At VSI, our patients are up and walking the same-day after their procedure. Most patients are able to start physical therapy within a few days of their surgery and return to light activity and modified work within a few weeks depending on their procedure.
Common aspects of recovery include:
- Gradual return to movement and daily activities
- Physical therapy to restore strength and mobility
- Follow-up visits to monitor healing and progress
It is also important for patients to understand what is normal during recovery and when to seek medical attention. Symptoms such as increased pain, signs of infection, or changes in mobility should be evaluated promptly.
Following post-operative instructions closely is one of the most effective ways to support healing and reduce the risk of complications.
Final Thoughts: Making an Informed, Confident Decision
Spinal surgery is an important decision, and understanding the potential risks is a key part of that process. While risks do exist, most are uncommon and can be effectively managed with the right approach to care.
By working with an experienced spine specialist, preparing properly for surgery, and following a structured recovery plan, patients can significantly reduce their risk and improve their outcomes. For many individuals, spinal surgery offers an opportunity to relieve pain, restore function, and return to a higher quality of life.
Taking the time to ask questions, understand options, and choose the right care team can help patients move forward with confidence.
Topics covered
About the Author
Featured Resources
Insights to Achieve a Pain-Free Life



