Flatback Syndrome
Understanding the Symptoms, Causes & Treatments of Flatback Syndrome
Reviewed by: Dr. Christopher Good, Dr. Colin Haines, Dr. Ehsan Jazini
What is Flatback Syndrome?
Flatback syndrome occurs when the lower back loses its natural inward curve, leading to a straight spine that becomes progressively flat over time. The human spine has four natural curves—two lordotic and two kyphotic —that work together to maintain balance and an upright posture. When viewed from the back, the spine should appear straight with the head centered over the pelvis. From the side, these curves form an ‘S’ shape, allowing the body to balance the head over the hips. Any imbalance in these curves can disrupt spinal alignment, forcing the body to adjust for upright posture.
In flatback syndrome, the decrease in lordosis leads to an imbalance that causes the patient to lean forward. Initially, patients may not notice significant changes, but over time, they may struggle to stand upright or experience worsening back and leg pain.
Flatback syndrome was initially noted in patients who had undergone scoliosis treatment using Harrington rods, common from the 1960s to the early 1980s. These rods straightened the spine but reduced its natural lordosis, leading to early disc degeneration below the fusion over time. While many patients initially did well, long-term issues emerged. Modern scoliosis implants and techniques now allow for multi-plane correction, reducing the risk of lumbar flatback syndrome. For more information on this condition, watch Dr. Good’s detailed explanation of flatback syndrome.
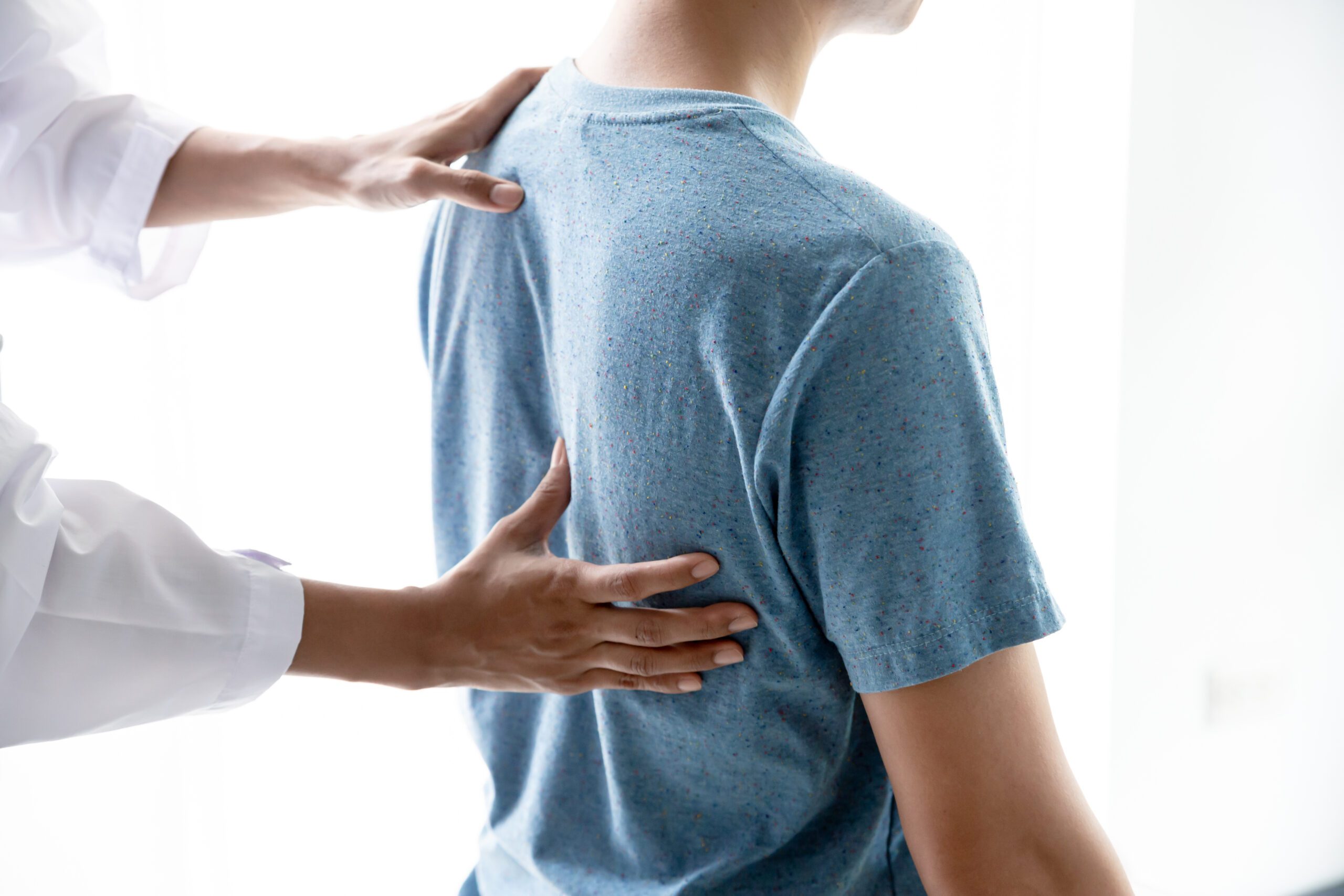
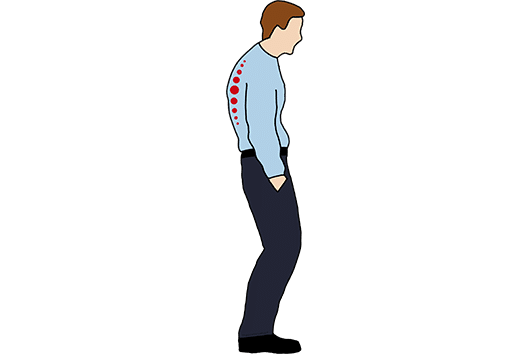
What Are Common Symptoms of Flatback Syndrome?
In flatback syndrome, the loss of normal lumbar curvature leads to spinal imbalance, causing the head to tilt forward and making it difficult for the patient to stand upright. To compensate, the body may tilt the pelvis and flex the knees or hips, which can result in muscle fatigue and pain. The severity of symptoms often correlates with the degree of curvature and difficulty in maintaining an upright posture. Patients might not immediately recognize the condition due to its gradual development.
Patients often seek help due to back or leg pain, difficulty with daily activities, or a sensation of falling forward. As symptoms worsen, they might notice worsening posture and may even begin using a cane or walking stick. This worsening is due to overcompensation, leading to increased muscular fatigue. Additionally, some patients with flatback syndrome may also have spinal stenosis, a condition where the spinal canal narrows, causing nerve-related symptoms.
When Should You Seek Treatment for Flatback Syndrome?
If you’re experiencing flat back symptoms or suspect a spinal issue, consult a board certified spine specialist promptly. Early diagnosis and treatment by a certified spine surgeon can improve your well-being and expand your treatment options. Addressing symptoms early is crucial for a successful recovery.
Persistent back or neck pain lasting more than 10 days should be evaluated by a spine surgeon, especially if accompanied by fever, loss of bladder control, or weakness/tingling in your limbs. These guidelines are based on decades of spine care experience, though individual cases may vary.

Still Unsure About Your Flat Back Condition?
Schedule a professional evaluation with VSI to receive a personalized diagnosis and expert guidance from a spine doctor. Opt for an in-person consultation for a comprehensive assessment.
What Are Common Causes of Flatback Syndrome?
Flatback syndrome now includes any decrease in lumbar lordosis causing symptoms, which can arise from conditions like:
Degenerative Disc Disease
The spine consists of vertebral bodies and discs. The discs are the soft tissue cushion and shock absorbers of the spine that allow for mobility. As a person ages it is normal that these discs will wear and tear which can cause asymmetric collapse. As the discs degenerate the spine begins to lean forward and lumbar lordosis will decrease. This can contribute to flatback syndrome and as a result patients may develop pain from their degenerative disc disease or from their spinal imbalance. Learn more about degenerative disc disease here.
Vertebral Compression Fracture
Compression fractures occurring within the spine often are due to an underlying condition called osteoporosis. This is a weakening of the bone and with increased stress a fracture can occur. Fractures change the alignment of the spine as fractures often include loss of height of the thoracic or lumbar vertebral body. This may occur in one or multiple bones throughout the spine resulting in flatback syndrome. Learn more about spinal fractures here.
Ankylosing Spondylitis
Ankylosing Spondylitis is a chronic inflammatory disease that affects the spine. Overtime it can cause stiffness, arthritis, and auto-fusion of the spinal vertebral bodies. This fusion causes the spine to be less flexible and can often lead to a hunched-forward posture. With this type of posture there is often increased thoracic kyphosis or decreased lumbar lordosis which can lead to lumbar flatback syndrome.
Failed Prior Surgery Syndrome
Lumbar flatback syndrome may develop in patients who previously were treated with a laminectomy or other spinal surgery to treat spinal stenosis and decompress the spinal canal and surrounding nerves. This procedure may lead to decrease in lumbar lordosis and in some cases spinal instability. Learn more about failed prior surgery syndrome here.
What are Common Treatments for Flatback Syndrome?
The goal of treatment for flatback syndrome is to improve patients’ symptoms and quality of life. Most conditions have two routines of treatment: nonoperative versus operative treatments. Non-operative, or conservative, treatments for flatback syndrome include an appropriate exercise routine which consists of aerobic fitness, weight bearing exercises, and core muscle strengthening. These all can help decrease a patient’s pain and improve bone strengthening which may decrease risk of osteoporosis. Spine-specialized physical therapy and spinal manipulation can be beneficial as well. Medications commonly are utilized to manage symptoms. In some cases Flatback syndrome can worsen pain associated with joint arthritis or a pinched nerve in which case spinal injections may be prescribed to provide relief. Many patients are able to stabilize their symptoms with these non-operative means and symptoms do not worsen warranting surgery.
At VSI, we help educate you on your spinal condition and discuss all treatment options, non-operative and operative, as well as risks and benefits. Flatback syndrome is a structural problem that often is associated with degenerative disc disease and spinal instability that may ultimately require surgical reconstruction. Surgery may be needed for certain patients that fail non-operative measures or whose deformity is worsening over time leading to other neurologic symptoms. Back symptoms often include pain, numbness, or weakness. The goal of surgical treatment of flatback syndrome is to restore lordosis, thus improving a patients overall alignment, quality of life, and stop progression of this spinal deformity.
Surgical recommendations are made after a comprehensive physical evaluation as well as review of all x-ray, MRI, and CT imaging with the spinal specialists. The goal is to provide excellent care to the patient by improving their symptoms and quality of life in the least invasive and safest possible way. Depending on the case, surgery to correct the deformity may involve a single or multiple approaches.
Your Path to Relief Starts Here
You may be dealing with ongoing pain, uncertainty, or a recent diagnosis. Our team specializes in treating flatback syndrome with both non-surgical and surgical options. The best next step is a personalized evaluation, with same-week appointment availability and no referrals needed.
Meet the Specialists Who Treat Flatback Syndrome
Our team includes board-certified spine specialists with extensive experience diagnosing and treating flatback syndrome. Each physician takes a personalized approach, combining advanced imaging, non-surgical therapies, and when necessary, surgical expertise to deliver the best possible outcomes.








