Endoscopic Surgery vs. Traditional Procedures
Key Takeaways
- Endoscopic spine surgery is a minimally invasive procedure performed through a small incision using a camera and specialized instruments.
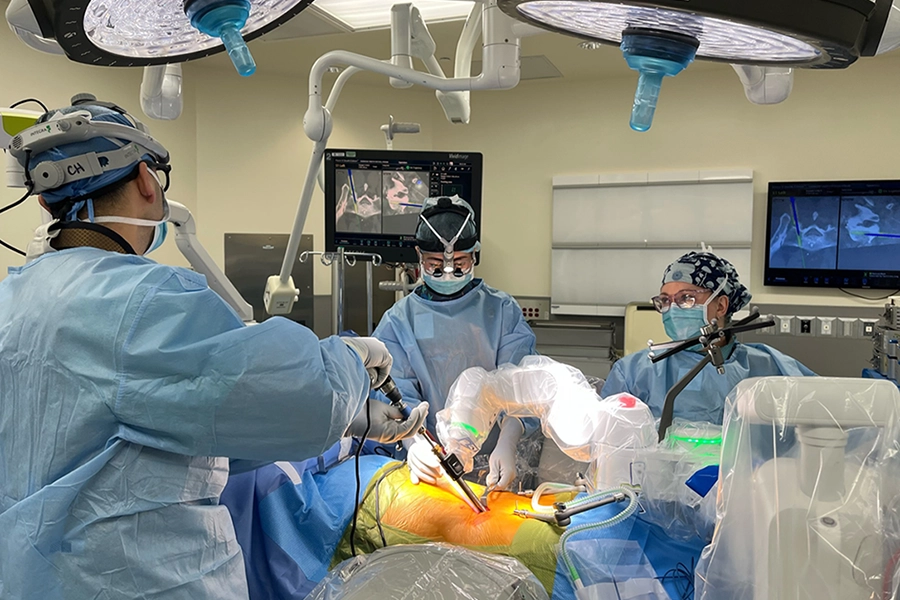
- Traditional spine surgery involves larger incisions and greater muscle exposure to directly access the spine.
- Endoscopic procedures typically result in less tissue disruption, reduced postoperative pain, and faster recovery.
- Traditional surgery may be necessary for complex, multi-level, or unstable spinal conditions.
- The best surgical approach depends on the specific diagnosis, severity of symptoms, and overall spine stability.
If you have been told you may need spine surgery, you may be wondering about the differences between an endoscopic procedure and a traditional open spine surgery. Both approaches are designed to relieve nerve compression, reduce pain, and improve spinal function, but they differ significantly in technique and recovery.
Endoscopic spine surgery uses a small incision and a camera-guided system to treat certain spine conditions with minimal muscle disruption. Traditional spine surgery, sometimes called open spine surgery, involves a larger incision and direct visualization of the spine. Understanding the differences between these approaches can help you make a more informed shared treatment decision in partnership with your spine specialist.
What Is Endoscopic Spine Surgery?
Endoscopic spine surgery is a minimally invasive procedure performed through a small incision using a thin tube and a high-definition camera. The surgeon inserts specialized instruments through this tube to access the spine without significantly disrupting surrounding muscles and soft tissue.
Because the procedure is camera-guided, it allows for targeted treatment of specific problem areas while minimizing tissue damage. In many cases, endoscopic spine surgery is performed on an outpatient basis.
Conditions commonly treated with endoscopic techniques include:
- Herniated discs
- Spinal stenosis
- Nerve compression causing radiculopathy or sciatica
The goal of endoscopic spine surgery is to relieve pressure on affected nerves while preserving as much normal anatomy as possible.
What Is Traditional Spine Surgery?
Traditional spine surgery, often referred to as open spine surgery, involves a larger incision that allows the surgeon direct visualization of the spine. Muscles and tissues are gently moved aside to access the affected area.
This approach has been used for decades and remains appropriate for many complex spine conditions. While it typically involves more tissue exposure than endoscopic techniques, it allows for comprehensive correction of structural issues.
Traditional spine surgery may be recommended for:
- Severe spinal instability
- Multi-level degeneration
- Advanced spinal deformities
- Cases requiring spinal fusion
Both endoscopic and traditional procedures aim to relieve pain and restore function. The choice between them depends on the specific diagnosis, severity of symptoms, and overall spinal stability.
Endoscopic Spine Surgery vs. Traditional Spine Surgery
| Category | Endoscopic Spine Surgery | Traditional Spine Surgery |
| Incision size | Small incision, often less than 1 inch | Larger incision for direct access |
| Muscle Disruption | Minimal muscle disruption using tubular system | Muscles gently retracted to expose spine |
| Visualization | High-definition camera-guided view | Direct visualization of the spine |
| Blood Loss | Typically less blood loss | May involve more blood loss depending on complexity |
| Hospital Stay | Often outpatient, same-day discharge | May involve longer hospital stay depending on complexity |
| Recovery Time | Generally faster recovery | Longer recovery depending on procedure |
| Postoperative Pain | Often reduced due to minimal tissue disruption | May involve more postoperative soreness |
| Conditions Commonly Treated | Herniated discs, certain cases of spinal stenosis | Multi-level disease, spinal instability, deformities, fusion procedures |
| Best For | Targeted nerve decompression with minimal structural correction | Complex structural correction and stabilization |
What Are the Benefits Of Endoscopic Spine Surgery
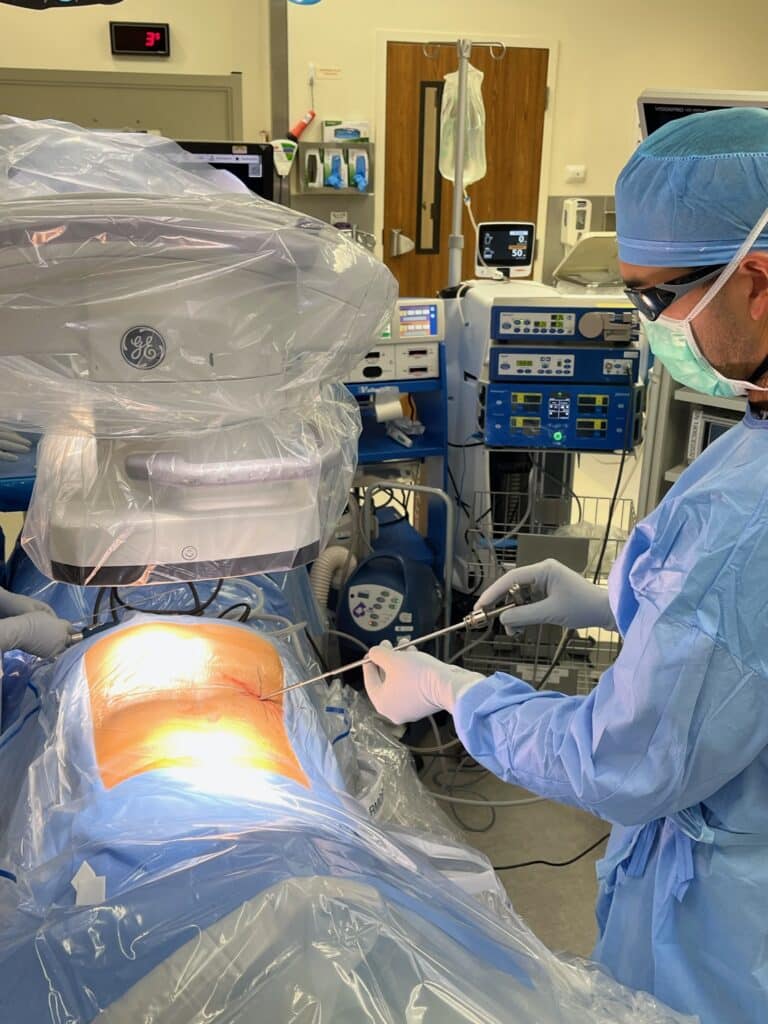
Endoscopic spine surgery offers several advantages for appropriately selected patients. Because the procedure uses a small incision and minimizes tissue disruption, recovery is often faster compared to traditional open spine surgery.
Common benefits may include:
- Smaller incision and minimal scarring
- Reduced muscle damage
- Less postoperative pain
- Lower risk of infection
- Shorter recovery time
- Often performed as an outpatient procedure
For patients with conditions such as herniated discs or certain cases of spinal stenosis, endoscopic surgery can provide effective nerve decompression while preserving surrounding structures.

Ready to Take the Next Step?
When Traditional Spine Surgery May Be Necessary
While minimally invasive techniques are effective for many conditions, traditional spine surgery remains essential in certain cases. More complex spinal issues may require a broader surgical approach to achieve stability or correct structural problems.
Traditional surgery may be recommended for:
- Severe spinal instability
- Multi-level degeneration
- Advanced spinal deformity
- Significant spinal fractures
- Cases requiring spinal fusion
In these situations, open surgery allows for comprehensive correction and stabilization of the spine. The goal is always to select the approach that provides the safest and most durable outcome.
Who Is A Candidate For Endoscopic Spine Surgery?
Not every patient is a candidate for endoscopic spine surgery. Ideal candidates typically have clearly defined structural issues that can be addressed through a minimally invasive approach.
You may be a candidate if you have:
- A single-level herniated disc
- Nerve compression causing leg pain or sciatica
- Mild to moderate spinal stenosis
- Symptoms that have not improved with conservative care
A detailed evaluation, including imaging and neurological assessment, is necessary to determine whether endoscopic surgery is appropriate.
Recovery Comparison: What Patients Can Expect
Recovery experiences after spine surgery vary based on the procedure performed and the individual patient. However, there are general differences between endoscopic and traditional spine surgery recovery.
Endoscopic Spine Surgery Recovery
- Often same-day discharge
- Smaller incision with minimal tissue trauma
- Faster return to light activity
- Shorter overall recovery timeline
Traditional Spine Surgery Recovery
- May require inpatient hospital stay
- Larger incision and more tissue exposure
- Longer recovery period depending on complexity
- May require more structured postoperative rehabilitation
Recovery expectations should always be discussed with your spine specialist, as outcomes depend on diagnosis, overall health, and adherence to postoperative guidance.
How A Spine Specialist Determines The Best Surgical Approach
Choosing between endoscopic and traditional spine surgery begins with a comprehensive evaluation. Imaging alone does not determine the need for surgery. Symptoms, physical examination findings, and overall spinal stability must align with imaging results.
A spine specialist will consider:
- The specific diagnosis
- Overall patient health and goals for recovery
- Number of spinal levels involved
- Degree of nerve compression
- Presence of spinal instability
The objective is to recommend the least invasive procedure that effectively addresses the underlying problem while maximizing safety and long-term function.
How To Decide Between Endoscopic and Traditional Spine Surgery
Both endoscopic and traditional spine surgery are designed to relieve pain and restore spinal function. The difference lies in surgical approach, tissue disruption, and recovery experience. For many patients, minimally invasive endoscopic techniques offer effective treatment with less postoperative discomfort and faster return to activity. However, traditional spine surgery continues to play an important role in treating complex or unstable conditions.
The most important step is obtaining an accurate diagnosis and discussing your options with a qualified spine specialist. A personalized evaluation ensures that the chosen surgical approach aligns with your condition, symptoms, and long-term goals.
Topics covered
About the Author
Featured Resources
Insights to Achieve a Pain-Free Life



