Working Together
Finding Solutions
Relieving Pain
The Ultimate Choice For Ultimate Spine Solutions®
Explore Our Resources
Empowering Our Patients Through Shared Knowledge
Blog
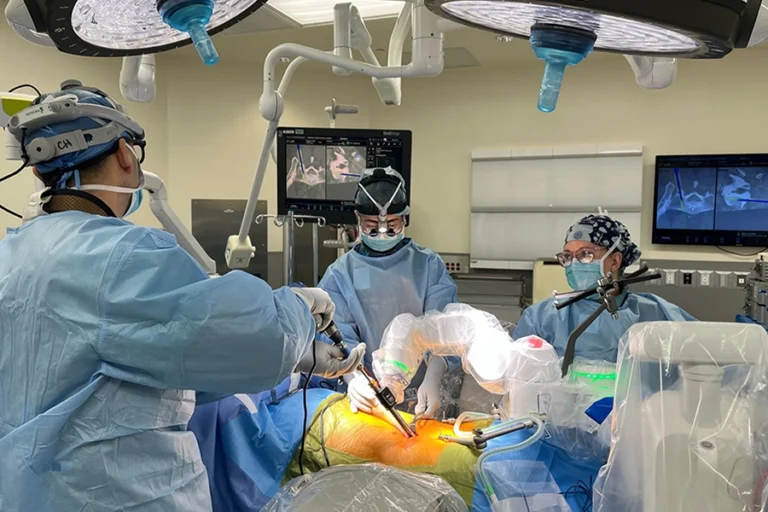
Endoscopic Surgery vs. Traditional Procedures
April 3, 2026
See More
Blog

The Back Pain Roadmap: How to Own Your Path to Recovery
March 30, 2026
See More
Blog

How Do I Know If I Need Spine Surgery Or If Conservative Care Is Enough?
March 26, 2026
See More
Blog

VSI Leads in Lumbar Disc Replacement Milestone in Mid-Atlantic Region
March 25, 2026
See More
Blog

How to Prevent Back Injuries While Playing Basketball
March 24, 2026
See More
Blog

What Are The Most Common Causes Of Back Pain In Adults?
March 19, 2026
See More
Blog
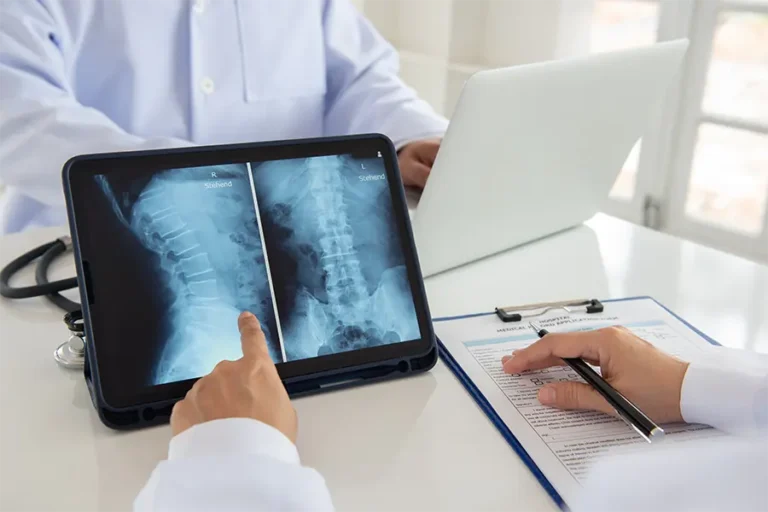
Do You Need an X-Ray, CT Scan, or MRI? How Doctors Decide
March 16, 2026
See More
Blog
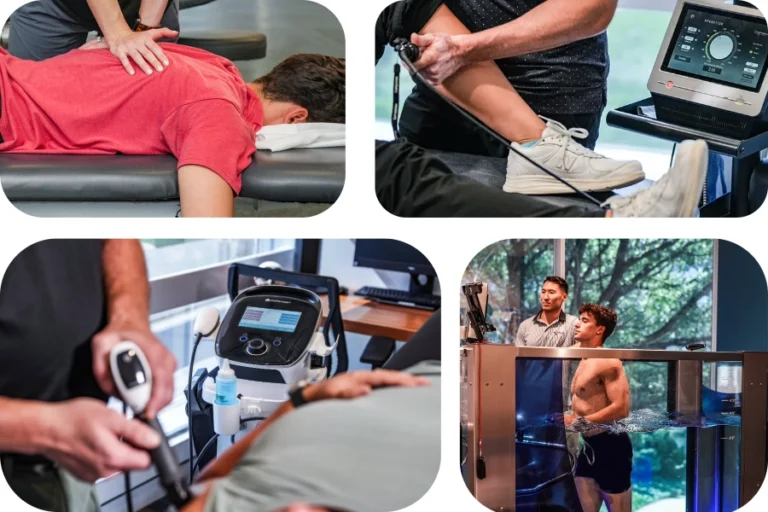
What Are Non-Surgical Treatments For Chronic Back Pain?
March 9, 2026
See More
Blog

Top 10 Things You Need to Know About Stem Cell Therapy
March 2, 2026
See More
Blog

Treating a Herniated Disc With Physical Therapy
February 26, 2026
See More
Blog

Top Warning Signs That Your Arm Tingling Could be at Risk for Permanent Nerve Damage
February 26, 2026
See More
Blog

How to Choose Between Disc Replacement and Spinal Fusion: A Patient Testimony
February 25, 2026
See More
Blog
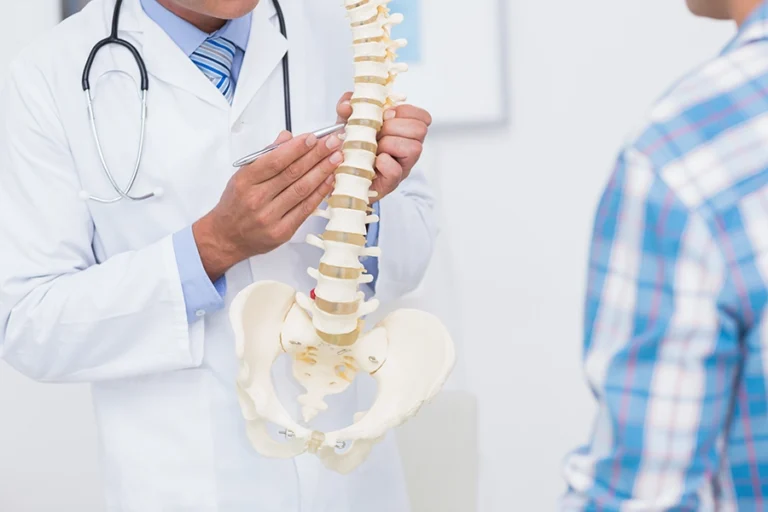
How Spine Specialists Determine the Best Treatment Plan for You?
February 17, 2026
See More
Blog
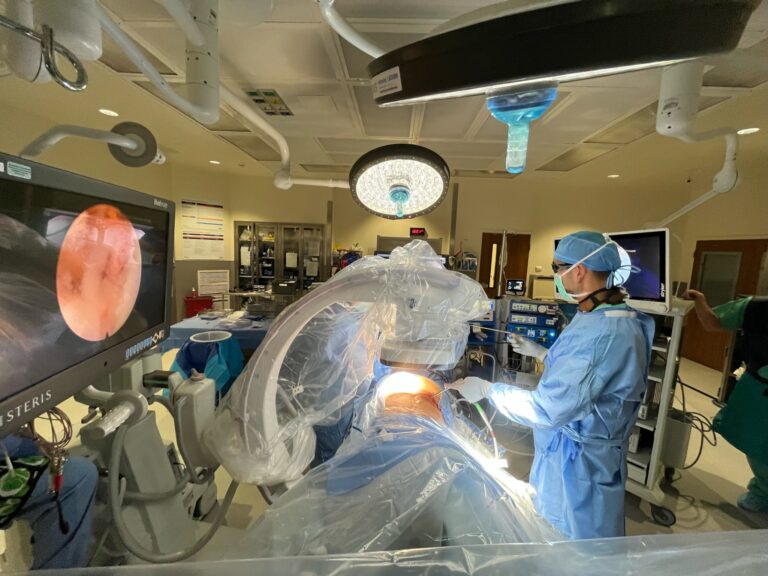
What Are the Benefits of Minimally Invasive Spine Surgery?
February 9, 2026
See More
Blog

5 Tips To Overcome The Post-Shoveling Aches And Pains
February 3, 2026
See MoreJoin The Conversation
#MyVSIVictoryStory
Before You Say Yes to Spine Surgery… Watch This
Which lumbar disc implant is right for me?
Basketball is harder on the spine than you might think!
Basketball & Back Pain: Slam Dunk Strategies to Stay Injury-Free
Is it ‘just a headache’? Or something more?
Why Women Suffer from Migraines and What Actually Helps
After Three-Level Disc Replacement, Nick is pain-free! #discreplacement #spinesurgery
Disc Replacement vs. Spinal Fusion: A Patient's Journey to the Right Decision
If you’ve ever wondered how to choose the right pillow, this video is for you!



